
Understanding Male Sexual Dysfunction in the 21st Century
A Comprehensive Guide to Erectile Dysfunction
Sexual health is a fundamental component of overall well-being, yet many men struggle in silence with conditions that profoundly impact quality of life, relationships, confidence, and mental health. Among these, erectile dysfunction (ED) is one of the most common and discussed issues — and increasingly so in today’s aging yet sexually active population.
As research advances and societal taboos soften, more men are seeking help and better treatments are becoming available. In this comprehensive guide, we explore what erectile dysfunction truly is, why it happens, common myths, the role of lifestyle, and modern approaches to diagnosis and management — spotlighting evidence-based care your audience can trust.
What Is Erectile Dysfunction?
Erectile dysfunction (ED) refers to the inability to achieve or maintain an erection sufficient for satisfactory sexual performance. It’s not a disease in itself, but a symptom that may result from physical, psychological, or mixed causes.
While occasional difficulty with erections is common, persistent issues (over 3 months) deserve medical evaluation.
How Common Is ED?
ED affects millions of men worldwide:
- Prevalence increases with age — up to 40% of men may experience some degree of ED by age 40.
- By age 70, nearly 70% of men report some degree of ED.
- However, younger men (20s–30s) are increasingly seeking help due to lifestyle influences such as stress, obesity, sedentary life, and mental health issues.
Despite its prevalence, many continue to suffer in silence due to embarrassment or stigma.
Causes of Erectile Dysfunction
The causes of ED are broadly categorized as organic (physical) and psychogenic (emotional/mental). Often, both coexist.
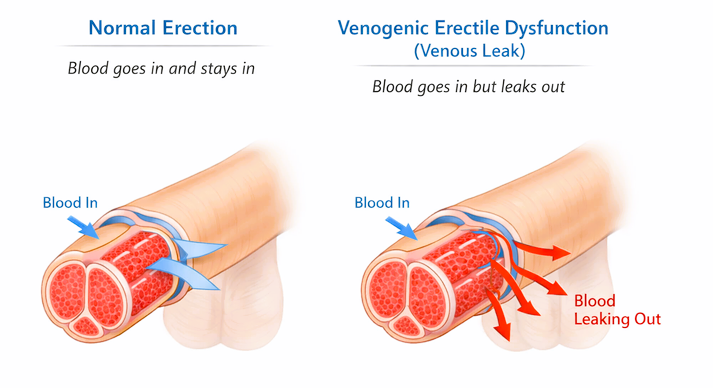
1. Vascular Causes
An erection depends on healthy blood flow to the penis. Conditions such as:
- Atherosclerosis (clogged arteries)
- High blood pressure
- High cholesterol
- Smoking
- Diabetes
- Obesity
can impair blood flow and lead to ED. In fact, ED may be an early warning sign of cardiovascular disease.
2. Neurological Causes
Nerves play a central role in erections. Damage or dysfunction — due to diabetes, spinal cord injury, multiple sclerosis, stroke, or surgery — can affect nerve signalling.
3. Hormonal Causes
Hormonal imbalances, especially low testosterone, can reduce libido and contribute to ED. Conditions such as hypogonadism, thyroid disorders, or chronic illness may be responsible.
4. Medications and Substance Use
Certain medications can affect erectile function, including:
- Antidepressants
- Antihypertensives
- Antipsychotics
Alcohol, smoking, and recreational drugs also interfere with sexual performance.
5. Psychological Causes
Stress, anxiety, relationship issues, depression, and performance anxiety are significant contributors — especially in younger men. Psychological ED is real and treatable with the right support.
Common Myths About Erectile Dysfunction
Despite growing awareness, misconceptions persist. Let’s bust some of the most common ones.
Myth #1: ED is Just a Normal Part of Aging
Truth: While aging increases risk, ED is not an inevitable consequence of getting older. Many men maintain healthy sexual function well into later years.
Myth #2: Only Older Men Get ED
Truth: Younger men are increasingly reporting ED due to lifestyle factors, stress, and psychological issues. Early evaluation can prevent long-term impact.
Myth #3: ED Is Always Psychological
Truth: Physical causes account for the majority of cases, especially in men over 40. Psychological factors may contribute — but should not be assumed without evaluation.
Myth #4: Medications Like PDE5 Inhibitors Are the Only Treatment
Truth: While medications (e.g., sildenafil) are effective for many, they are not the only treatment. Lifestyle changes, vacuum devices, hormone therapy, counselling, and advanced urological procedures can all play roles.
How Is Erectile Dysfunction Diagnosed?
A thorough diagnosis is crucial — it guides treatment and identifies underlying health issues.
Clinical History
Your doctor will discuss your symptoms, medical history, medications, lifestyle, and psychological health.
Physical Examination
A physical exam looks for signs of underlying disease — such as cardiovascular problems, hormonal imbalance, or nerve damage.
Laboratory Tests
Blood tests may assess:
- Blood glucose (for diabetes)
- Lipid profile
- Testosterone levels
- Thyroid function
Specialized Tests
When needed, urologists may perform:
- Doppler ultrasound to check penile blood flow
- Nocturnal penile tumescence tests to distinguish physical vs psychological ED
- Injections or pharmacologic tests to evaluate vascular response
Modern Treatment Options
Treatment is personalized. What works for one patient may not work for another. The approach depends on cause, severity, overall health, and patient preference.
1. Lifestyle Modification
Simple changes can have a powerful impact:
- Maintain healthy weight
- Control blood sugar
- Regular exercise
- Quit smoking
- Limit alcohol
- Manage stress
These changes improve overall health and erectile function.
2. Oral Medications (PDE5 Inhibitors)
Medications like sildenafil, tadalafil, and others improve blood flow to the penis.
- Effective for many men
- Well-studied and widely used
- Require medical evaluation beforehand
However, not all men can take them (e.g., nitrates for heart disease).
3. Vacuum Erection Devices
These devices create suction to draw blood into the penis and maintain an erection using a constriction band. They’re effective and safe in many cases.
4. Penile Injections & Suppositories
Medications such as alprostadil can be injected or inserted to produce an erection. They are alternatives when oral medications fail or are unsuitable.
5. Hormone Replacement Therapy
If low testosterone is diagnosed, hormone therapy may be recommended under careful medical supervision.
6. Penile Prosthesis Surgery
For men who do not respond to conservative measures, penile implant surgery provides a reliable and long-term solution. Urologists trained in reconstructive techniques can tailor prostheses to patient needs.
The Role of Reconstructive Urology in Sexual Health
Sexual dysfunction often reflects broader urological or systemic disease.
Specialists trained in reconstructive urology — like Dr Dilip Kumar Mishra — manage complex conditions such as:
- Peyronie’s disease (penile curvature)
- Post-prostatectomy ED
- Trauma-related sexual dysfunction
- Urethral strictures affecting sexual function
Surgical expertise, including laparoscopic and minimally invasive techniques, enables advanced management where conservative treatment doesn’t suffice.
Psychological Factors and Central Support
Medicine and surgery address the physical aspects — but sexual health is more than physiology.
Couples therapy, sex therapy, and cognitive-behavioural therapy have proven benefit, especially when performance anxiety or emotional factors contribute. Integrating psychological support with medical care yields the best outcomes.
Lifestyle and Prevention — The Hidden Power
Prevention and optimal sexual function go hand in hand. Encourage patients to see ED as an opportunity — not an embarrassment — to improve overall health.
Key preventive steps include:
✔ Cardiovascular fitness
✔ Healthy diet (Mediterranean-style)
✔ Smoking cessation
✔ Stress reduction
✔ Sleep optimization
✔ Regular health check-ups
These approaches decrease ED risk and improve life quality.
When Should You See a Urologist?
A primary care physician may start evaluation, but referral to a urologist is recommended when:
- ED persists beyond 3 months
- Symptoms are severe
- There’s sudden onset
- Associated with penile deformity
- Accompanied by pain or trauma
- Conservative treatment fails
A specialist can offer advanced diagnostics and a comprehensive, personalized treatment plan.
Breaking the Silence: It’s OK to Ask for Help
Sexual health affects emotional well-being, relationships, and self-esteem. Men often delay medical help due to embarrassment or misconceptions — but ED is rarely “just in the mind,” and effective treatments exist.
If you’re experiencing sexual difficulties, you don’t have to suffer in silence. Early evaluation leads to better outcomes — and may reveal important insights about your overall health.
Conclusion: ED Is Treatable — And You’re Not Alone
Erectile dysfunction is common, multifactorial, and treatable. From lifestyle measures and medications to advanced urological interventions and psychological support, modern medicine offers a spectrum of effective options.
Whether you are a patient seeking answers or a partner supporting someone you care about, understanding the facts — and dispelling myths — is the first step toward improvement.
At its core, ED is not a failure — it’s a signal. With the right expertise, empathy, and evidence-based care, sexual function can often be restored and quality of life significantly improved.

